Virtual Reality in Occupational Therapy: Interview with Blandine Le Mené
The career of Blandine Le Mené, a private occupational therapist, and her use of virtual reality How can virtual reality…
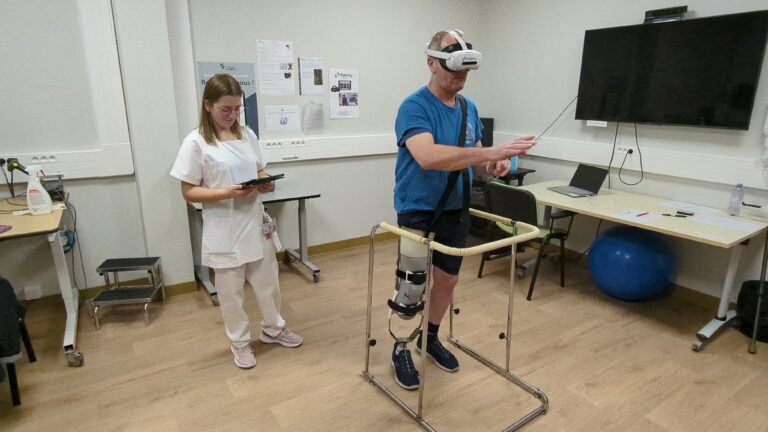
Virtual reality vestibular rehabilitation is an innovative approach for practitioners confronted with vertigo, balance disorders and dysfunctions of the proprioceptive system. Whether you work in a private practice, in an ENT department or in a rehabilitation centre, you know the complexity of these pathologies and the limits of traditional protocols. This article presents how virtual reality is transforming vestibular care, and why more and more physiotherapists and occupational therapists are integrating it into their practice.
The vestibular system is the set of structures in the inner ear responsible for balance, spatial orientation and stabilization of the gaze. It constantly works in coordination with vision and proprioception to keep the body in balance.
When this system is disrupted—after head trauma, benign paroxysmal vertigo (BPPV), vestibular neuritis, or ear surgery—the patient presents with disabling symptoms: rotational vertigo, gait instability, nausea, and severe anticipatory anxiety. Indeed, the latter constitutes a major obstacle to rehabilitation: the patient avoids triggering situations, which maintains the vicious circle of deconditioning.
Certainly, the classic protocols (Épley manoeuvres, Cawthorne-Cooksey exercises) are effective. However, they have limitations: difficulty in reproducing precise stimulations, lack of objective feedback on progress, and low patient engagement over time.
Virtual reality vestibular rehabilitation is based on a simple principle: exposing the patient to controlled visual and postural stimulation, in a safe environment, in order to force the central nervous system to recalibrate its processing of balance information.
In concrete terms, the patient wears a VR headset that offers vestibular habituation exercises — environments with optical flows, moving scenes, virtual movements — while his body remains still or performs guided movements. Thus, the practitioner adjusts the nature and intensity of the stimuli in real time from his control interface.
The therapeutic mechanisms at play:
Moreover, according to Lee et al. (2025), virtual reality-assisted vestibular rehabilitation shows comparable efficacy to conventional protocols, with superior improvement in physical domains and confidence in movement in patients with acute unilateral vestibulopathy.
Virtual reality vestibular rehabilitation is aimed at a wide spectrum of clinical situations. Among the main therapeutic indications covered by the H’ability device:
A typical session with the H’ability device lasts between 15 and 30 minutes. It takes place as follows:
1. Initial assessment — first of all, the practitioner selects the protocol adapted to the patient’s profile: type of vestibular pathology, stage of rehabilitation, tolerance to visual stimulation.
2. Installing the headset — Next, the H’ability device is based on the Pico 4 Enterprise headset, which is self-contained and cable-free. It takes less than 2 minutes to get started. Mixed reality mode is enabled for sensitive patients: the patient sees his or her real environment enriched with virtual elements, which significantly reduces the risk of nausea.
3. Immersive exercise — the patient then performs the exercises in a sitting or standing position depending on their condition. The proposed scenes (optical flows, moving environments, cognitive and postural dual tasks) are gradually adapted to difficulties.
4. Real-time monitoring – in parallel, the practitioner observes on his tablet the movement data, the scores obtained and the evolution compared to previous sessions.
5. Debriefing — finally, the practitioner and patient analyze the results together. This feedback moment reinforces motivation and therapeutic compliance.
Some vestibular patients are particularly susceptible to VR-induced nausea. However, the mixed reality mode integrated into the H’ability device reduces this risk by maintaining the patient’s real visual cues. For this reason, prior evaluation is recommended for patients with a history of severe motion sickness. To learn more, see our article on cyber kineticosis in virtual reality.
“Handtracking makes the exercises more fun and interactive, which makes the sessions more effective. We have seen people in pain mobilize their limbs, when they did not do so outside of virtual reality. »
— Baptiste Mourant, occupational therapist at the Les Capucins Rehabilitation Centre (Angers)
What is vestibular rehabilitation in virtual reality?
Virtual reality vestibular rehabilitation consists of exposing the patient to controlled visual and postural stimulations via a VR headset, with the aim of recalibrating the central nervous system after vestibular dysfunction. In other words, it complements traditional protocols by providing an immersive environment, objective feedback and better patient compliance.
What vestibular disorders are treated by virtual reality?
The main indications are: BPPV, vestibular neuritis, post-surgery of the inner ear, post-traumatic balance disorders and vestibular migraine. In addition, VR is also effective in preventing falls in seniors with postural deconditioning.
Can virtual reality cause nausea in a vestibular patient?
This is a risk to be assessed on a case-by-case basis. Nevertheless, the H’ability device integrates a mixed reality mode that allows the patient to see his or her real environment during the session, thus significantly reducing the risk of cyberkinetosis. Preliminary evaluation is therefore recommended for patients with a history of severe motion sickness. It should be noted that the H’ability device is not indicated for patients with severe behavioral disorders.
Is the VR headset suitable for all vestibular patients?
It is suitable for the vast majority of adult patients with stable vestibular pathology or in the compensatory phase. On the other hand, a prior clinical evaluation allows the protocol to be adapted to each profile. The progression of the exercises — in difficulty and intensity of the stimuli — is thus entirely controlled by the practitioner.
How many sessions does it take to see results?
Vestibular rehabilitation generally requires 6 to 12 sessions depending on the pathology and the patient’s condition. In practice, the first improvements in balance and reduction of dizziness are often observed from the 3rd or 4th session. This is why the regularity of the sessions is decisive for the effectiveness of the protocol.
References:
The career of Blandine Le Mené, a private occupational therapist, and her use of virtual reality How can virtual reality…
Returning to sport after an injury is one of the most delicate stages of the treatment journey. Only 24% of…
Mixed reality, or MR, is one of the most promising innovations for rehabilitation. More advanced than classic virtual reality for…
Parkinson’s disease is a progressive neurodegenerative disease that affects nearly 200,000 people in France. Beyond drug treatment, rehabilitation plays a…